
NOTE: This blog was just put back online on Aug. 29, 2021
In March of 2015 I posted the following “health information” on my blog as a “case study” on a complex autoimmune health problem I’ve been battling since 2009. I am hoping by sharing it here, that might lead to answers and a sort of “open source medical cure.” By 2018, without any answers and an HMO plan which was restricting my getting those answers, I took it “off-line” because I felt it might lead to biases in work and personal/social activities. Then on Aug. 29, 2021, with the world still in the grips of the Covid19 pandemic, with restrictions & delays in many everyday medical services, I decided to put this back “online” as I think I am getting close to receiving a “diagnosis.” There is also a parallel between my autoimmune case study, and the Covid19 pandemic, in that both are centered around autoimmunity, and each of us must be healthy enough to produce “antibodies” from either natural immunity after a Covid19 infection, or after vaccination by one of three available Covid19 vaccines. As I earlier worked with “infectious diseases” (AIDs, TB, staff, hepatitis) in earlier nuclear (owned & operated Certified Nuclear Imaging” from 1982 – 1992), have accrued a great deal of expertise in public health from my public health work with CNS shunts, and have spent the last 10 years learning “auto-immunity” trying to solve my own autoimmune disorder – I really feel like I have some expertise or insights to offer in Covid19.
The photo at top is me pictured two days after my 5th brain shunt surgery (Feb. 1998) for hydrocephalus. My own CNS shunt complications led to me becoming a patient advocate, neuroscientist, and inventor of the DiaCeph mHealth Test for hydrocephalus that I’ve used to co-direct my last 8 brain shunt surgeries, and provide consults and related patient care information around the world. I also became involved in music therapy, and eventually “drumming,” or drum circles, and then a drum circle facilitator.
In 2009, I began to experience muscle cramping which began to cause blood in the urine, and partial kidney failure, after the rigorous exercise of some of my drumming events. Two years later, I was diagnosed with Hashimoto’s Thyroiditis, fatigue and worsening muscle complaints, dry eye, rashes, anemia, eosinophilia, bone pain, and in 2015 “meningeal enhancement” on my MRI brain scan with Gadolinium. The MRI finding was eventually diagnosed as “pachymeningitis,” which is non-infectious inflammation of the meninges, or the lining covering the brain and spine, and I was placed on corticosteroids (primarily prednisone). I also live with a VP shunt for hydrocephalus since 1992. The actual cause or diagnosis of my pachymeningitis has yet to be identified. Further below is my 2015 CSF lab report, and MRI brain scans that evidence dura enhancement and pachymeningitis. I now have NEW 2021 MRI imaging results and lab work after being off prednisone for 18 mo, plus upcoming appointments with specialists that I think will put me closer to a diagnosis. MRIs of my brain, cervical, and thoracic spine with Gadolinium show diffuse “meningeal enhancement” down into my thoracic spine. This is thought to be from “chronic intracranial hypotension” from overdrainage of my CNS shunt for hydrocephalus. But I am skeptical of this as the diagnosis as I’ve experienced overdrainage in the past, and know how to identify and manage it with a programmable shunt. The biggest challenge I think, is diagnosing an underlying autoimmune disorder and noninfectious meningitis in the presence of hydrocephalus. I will share more in the coming weeks.
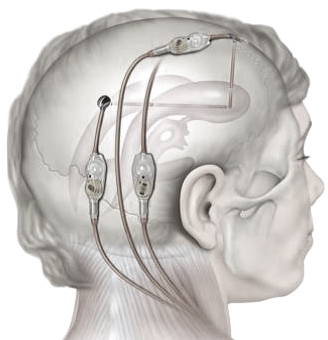
My hydrocephalus history spans 1992 to present with a total of (12) CNS shunt operations, or revisions. The shunt complications, poor outcomes, and confusion in my care during those first few years led to my doing field research, activities as a patient advocate, and then authoring of this important 1996 Food & Drug Administration petition on anti-siphon shunt devices that led to the 1999 FDA STAMP Conference in Bethesda, Maryland. In the interim two year period that FDA reviewed my petition, I researched and designed my DiaCeph mHealth Test shunt monitoring system, and was bestowed the title of “scientist” for my efforts without attending school again for a masters or PhD degree.
As for my medical patient experiences, along with 12 surgeries and hundreds of shunt malfunctions, accidental reprogramming of my shunts, and numerous embarrassing and personal challenges, I’ve also undergone about 70 brain scans, half or more of those being CT scans with the associated radiation exposure. I’ve also underwent 4 or 5 procedures where foreign substances (dye & radio-tracers) were injected into my shunt system that can lead to infection and CNS complications.
Unfortunately, I could never get the requisite funding or support for my DiaCeph Test and DiaCeph Inc. startup, which would have enabled early reporting and sharing of data on shunt devices. My company plans were to also pursue “brain apps” which I had been researching, and minimally available on PDAs at that time. Without availability of my DiaCeph Test, it took some of the best neurosurgeons 16 years (2008) and 6 revisions to get the swelling on my brain returned to normal. In 1998, I shared my DiaCeph Test to Dr. Eldon Foltz, chair of the Dept. of Neurosurgery at the University of California at Irvine. From 1998 on, I used the DiaCeph Test’s paper forms & instructions for pre & post surgical diagnostics and status assessment. Since 2009, I have been providing shunt monitoring consults to patients and families around the world. Today also health and safety failures with CNS shunts continues to be a considerable problem.
My primary health issue today surrounds a yet to be diagnosed autoimmune disorder and chronic meningitis. It may have been “triggered” by numerous invasive procedures and stresses of my shunt revisions. Or it may be a worsening of a childhood disorder tentatively diagnosed as a peripheral neuropathy in 1980. Without good health insurance, solving this riddle has been elusive. Since 2009, my complaints have worsened and become more systemic without any diagnosis or effective treatment or pain management. My present insurance is a United Healthcare managed care plan, and they have put up barriers to care, causing me to file (4) “grievances” between 2012-2015, and I have also put my privacy at risk in this case study.
Feb. 7, 2017 UPDATE:
In this most recent update, I share a new Rx order for a more detailed CSF (cerebrospinal fluid) lab test. I was given this order in early Dec. 2016, but am yet to undergo the labs due to uncertainty over discontinuing Adaptogens and Nootropics supplements which have brought some relief in my complaints in recent months. In late 2015, I authored this Blog on Nootropics from my research. My initial goal was to replicate the cognitive benefits I experienced in 2015 from the Exelon Patch drug. And secondly, to see whether Adaptogen herbs might bring relief to my pain and fatigue. And both did to some degree.
My recent improvement in late Dec. 2016 led to raising the pressure setting on my Certas hydrocephalus shunt valve – from a setting of “3” to “4.” This change is important as my shunt setting had earlier been down to “2” for 3-4 years due to low intracranial pressure (ICP) from the dura (brain) inflammation. I am yet to update my Nootropics blog with my latest findings, but I expect to over the next month. Below, are three images of my current supplements. The 2nd image also denotes via text: Modafinil, Prednisone, and Synthroid – which are drugs that produce “systemic” changes in the body. More recently, I’ve also added Alpha GPC to my daily Nootropics.



As much as the above supplements provided some relief in my complaints, I am uncertain which ones provided the benefit. I have also just learned that several of the Adaptogens, specifically Panax Ginseng and Ashwaghanda, also boost immune function, and this in turn diminishes the effect of my Prednisone. I could not get a definitive answer on Maca Root. I had noticed intermittent relief & worsening pain over the last 3 months. This new information by Natural Medicines then explains it. And I need to learn which of the above supplements I need to discontinue prior to this next round of CSF labs, and for how many weeks. And after this test, I need to decide what combination of Prednisone and supplements would be best. Should there be a definitive diagnosis, that will be very helpful.
Below, is the order slip for this next round of CSF labs. As I stated, it is unclear which supplements & prescription drugs I should be off, and for how long (Q1). This likely includes Prednisone, Panax Ginseng, and Ashwaghanda, and perhaps others. I have delayed this test due to these outstanding questions, and in transitioning off, and back on, these supplements. Perhaps I shouldn’t even be on them? I’d also like to know if there are additional CSF tests to add to this Rx list (Q2)? A CSF sample can be readily accessed thru my shunt reservoir under my scalp with relatively low risk.

This concludes my Feb. 7, 2017 status update. I am encouraged. The biggest abnormality in my CSF cell count (2015) is a low WBC count (lymphocytopenia). My protein level was also elevated. And I have had an elevated blood absolute eosinophils count and low “RBC” levels for much of the last 5 years. But my Oct. 2016 blood labs were in the normal range – after 10-12 months of supplements. I have also obtained and reviewed new autoimmune studies relating to dura inflammation and CSF testing which are applicable to my case history. Earlier in 2016, both my muscle biopsy & genetic tests (UCLA) were negative.
History Continued:
The history of my current neuromuscular complaints (beyond my earlier controlled peripheral neuropathy) arose in 2009 with hematuria (myoglobinuria) and subsequent kidney failure following a 4-hour drumming event, initially diagnosed as rhabdomyolisis. At that time, I had little neuromuscular cramping or pain other than in my back and lower legs that were well controlled with exercise. After this 2009 hospitalization, my cramping and extremity pain turned and global fatigue and affected the use of my hands and physical activities, with episodes of myoglobinuria and cramping occurring at lower thresholds of activity.
In late 2011 I was diagnosed with Hashimoto’s thyroiditis, thought secondary to an autoimmune disorder. And since 2012, my complaints have escalated to considerable global pain and cramping, fatigue, cranial nerve palsies, low intracranial pressure (ICP), and cognitive challenges beyond that of hydrocephalus. In late 2015, the dura inflammation was diagnosed as pachymeningitis (UCLA) esp after my positive response to Prednisone (SEE MRI below where ventricles collapsed after Prednisone). In my Oct. 13, 2016 update, I added photos and discussion regarding my childhood health issue, where drooping on the left side of my face/mouth can be seen as early as age 11.
I take a low dose Prednisone (2.5mg ea other day) that slightly helps with pain and cramping. Due to effect of Prednisone on my ventricle size (hydrocephalus), this has to be closely monitored with my DiaCeph Test & MRI brain scans, with adjustments in the pressure setting of my programmable Certas shunt, which has also been recalled and not yet revised. I need a mHealth app to sort this all out.
In January 2016, I hospitalized for a sepsis infection felt due to Methotrexate and Azithioprine I had been on for a few months. It did resolve much of the dura inflammation on MRI brain scan with Gadolinium, lending support to the pachymeningitis diagnosis. And in May 2016, I underwent a muscle biopsy with consideration of a mitochondrial disorder. However, the muscle biopsy was negative. There was some question if I was off Prednisone long enough.
In Oct. 2016, a brain tissue biopsy was proposed. But my neurosurgeon has advised against it. In my research, I focused on my abnormal CSF cell count, particularly my very low lymphocyte count seen in the image below. My other WBC counts are moderately elevated. Many CNS disorders today are identified in CSF counts. Please comment at bottom if you have familiarity with disorders that might cause this type of CSF count.

Here’s what I need as of Feb. 7, 2017:
- In Aug. 2016 I was referred to an immunologist at UCI Medical Center. But my United Healthcare plan denied it, instead referring me a rheumatologist with Great Newport Physicians, who ordered a brain tissue biopsy and this new CSF lab tests. At this time I need: a) A list of medications & supplements to be OFF, and for how long for the CSF lab test. b) Recommendations of any additional tests that might help identify my disorder.
- I would like access to medications like the Exelon Patch (memory drug) & pain medications that support quality of life. Trash-men, freeway workers, and government union workers can get these medications. Denying these medications to others in need is a form of inequality & discrimination.
- I would like scientists and FDA to convene & expedite development of new safer CNS shunts, an ICP sensor and/or mobile app like my DiaCeph Test to monitor 24/7 CNS shunt function in hydrocephalus, and put an end to health and safety dis-information with CNS shunt technology.
- I would like NIH to convene scientists and address the epidemic of PTSD (post traumatic stress disorder) and SPD (sensory processing disorder) – and make recommendations for testing, treatment, and accommodations in public places, and help mitigate the practice of loud audio media (TV/radio) in commercials – that affects 10-20 percent of Americans.

Exelon Patch memory drug by Novartis
Use of the Exelon Memory Patch really is an accessibility issue in the presence of neurological disorder or brain injury. I doubt any health plan would deny an accommodating aid to a blind person or individual confined to a wheelchair. But, brain disability, it has no voice!
As for my United Healthcare health plan, between 2012 and 2014, I had to file five (5) appeals & grievances in order to receive treatment, that led to unnecessary delays. I have also suffered a number of medical errors, the most significant recent one was misdiagnosis of dura inflammation on my Feb. 2012 MRI brain scan with gadolinium. The inflammation wasn’t discovered until February 2015. Then it took another six months for Prednisone to surprisingly collapse my ventricles. And then a ton of research and advocacy on my part for my UCLA neurologist to make the diagnosis of pachy meningitis. And it is only a partial diagnosis.
Pachy meningitis is inflammation of the brain usually secondary to another disorder, which, in most cases, is an autoimmune or neuromuscular disorder. It was my innovative mHealth efforts after the collapse of my ventricles (hydrocephalus, treated w/ CNS shunt) in June 2015 while on Prednisone, that led to the pachymeningitis diagnosis. I am hoping my case study blog can also become a teaching experience on mHealth.
March 21, 2016 Status Update
Currently, I am awaiting scheduling of a muscle biopsy for evaluation of myositis and mitochondrial disorder. However, it is being complicated by delays by my United Healthcare HMO plan who is issuing the authorization. This likely would have been done back in 2012. I am taking a low dose of Prednisone which helps with cramping and pain. But, I will have to be off this for 4-6 weeks before the muscle biopsy.
It was on Dec. 28, 2015, that I learned dura inflammation was present back on my Feb. 2012 brain scan – but was missed by the radiologist. It was serendipity and my innovative MRI mHealth method of brain scan images I exported to my Nook tablet, that helped make these discoveries possible.
My mHealth Display Method of CT/MRI Images on LinkedIn

My MRI/CT mHealth Method: Since 1999, I’ve gotten CDs of my CT/MRI brain scans. Prior to that, I obtained copies on film and would photograph them. As of 2016, I’d undergone about 60-70 brain scans, along with 12 brain shunt surgeries. It was about 2002 that I created this mHealth display method to feature my own brain scans in my Shunt Selection Study on my web site for hydrocephalus. This method allows for review of 1000s of CT & MRI images by placing critical images in a chronoligcal sequence for review. Use of these displays would also reduce interpretation medical errors.
I first create folders on my PC for each interested CT or MRI series. Then I export the images as JPEGs into the respective folders using the media software program included in the radiology CD disc. Next, I review, select, and label the relevant images and copy them into another folder, where they can be arranged in chronological series and be viewed side by side. This format makes interpretation more scientific, and minimizes the possibility of human (visual) error from misinterpretation.
This method is particularly important in hydrocephalus care – where it is common to have dozens of studies and 1000s of images to be reviewed. This mHealth display method benefit radiologists, neurologists, and neurosurgeons involved in hydrocephalus care. This method also allows for more detailed evaluation of shunt settings, shunt performance, and shunt malfunction. I have also put these mHealth advances to good use in my hydrocephalus consults and shunt monitoring services linked below:
Hydrocephalus and NPH Shunt Monitoring Consults
Once I have assembled the critical MRI/CT Images Folders, I can easily sync and copy the folders onto my phone and tablet. Then when I see my neurosurgeon or neurologist, I’ve got all of my brain images neatly organized for review and discussion.
It was during my Dec. 28, 2015 visits to discuss my post Methotrexate & Prednisone MRIs, that each (serendipitiously) observed pachy meningitis was present on two Feb. 2012 MRI images w/ Gadolinium I had in the display. I included them when I published this blog in April 2015, but didn’t think the images were comparible as they were from different series. These specialists see these studies every day and picked up on the abnormalities right away. I’m just the mHealth inventor! But I regularly get asked to demo these displays.
I’ve really been deteriorating since 2012, haven’t been able to keep up with drumming and other responsibilities because of widespread cramping, pain, and fatigue. On many days, I did not get out of bed until 11 a.m. or noon, and other days I’d return to bed by early afternoon. I wasn’t able to share this for fear of losing the little work I was doing.

My neuromuscular challenges are in addition to challenges I’ve faced with my CNS shunts, where manufacturers were aware of safety issues, but failed to notify FDA. I know this because I became a patient advocate in 1995 and keep abreast of shunt issues. Failing to report shunt safety issues has been the rule, which I discuss later in this blog.
Currently I am awaiting scheduling of a muscle biopsy for the progression of complaints that seem related to a neuro-muscular disorder for which a biopsy was done in 1980. I also seek answers in these Healing Arts (blog) and Alternative Medicine (blog). UCLA Medical Center has two healing arts centers: The Norman Cousins Center for PsychoNeuroImmunology and the Mindful Awareness Research Center.
My 1992 Auto Accident – Diagnosis of Hydrocephalus

The MRI brain scan below was taken one month post trauma and reveals very large ventricles suggestive of longstanding ventriculomegaly – which likely worsened with the accident and concussion. It’s speculated that I may have had a very small subdural bleed on my right side causing further ventricular enlargement because my right ear drum was “red” on exam one day following the accident. No brain scan was performed. It wasn’t until 4 weeks later, when I developed severe headaches and marked confusion (didn’t know what side of the street to drive on), that a brain scan was done (1992 below). This accident was caused by a 17 year who ran a red light, prior to mobile phones. I was returning home from volunteer duties at the 1992 Great American Race awards banquet, where I had been on a chamber arts committee to raise money for Costa Mesa arts. As they say, “No good deed goes unpunished!”
In support of hydrocephalus, and my yet diagnosed neuromuscular disorder, I would like to share my Hydrocephalus Blog for Rare Diseases Day. Seems one’s duties never end!

Earlier in 1980, I had been diagnosed with an unspecified neuromuscular disorder that had been causing me considerable pain and weakness in my legs and back, that I had been battling since my early teens. With a poor prognosis not offering much hope, I delved into the healing arts which proved to provide a great deal of relief. It even led to skills as a medical intuitive, corroborated in my clinical imaging work. This Healing Arts Blog documents these unusual 1981 healing experiences. I had a remarkable remission of this neuro-muscular disorder and managed it quite well until about 2009, when I began to develop unexplained hematuria/kidney failure with urine pictured below when I undertook rigorous exercise and hand drumming.

By 2012 these bouts had significantly worsened and were occuring at lesser levels of exercise and drumming. I would load up (hydrate) with water and Gatorade before, during, and after drumming and physical activities. But as you can see in the photo, sometimes I couldn’t overcome the effects of this disorder with hydration. On two occassions, I was hospitalized. On perhaps 12 or 15 others, I self treated at home with fluids, urine measurements, and photos like you see above for my records. Today, these complaints are thought connected to my pachy meningitis and Hashimoto’s thyroiditis via an anto-immune or metabolic disorder.
Dura Enhancement = Pachy Meningitis
In February 2015, a CSF culture was done and revealed marked abnormalities in WBCs suggestive of inflammation, but not for infection (SEE JPEG report further below). My neurosurgeon felt it represented chronic shunt overdrainage and intracranial hypotension. But neither my clinical history, nor above-sized ventricles on my brain scans, coincided with chronic overdrainage as reported in the medical literature.
My case study then seemingly began to surround these findings of diffuse dura enhancement – suggestive of either chronic non-infectious meningitis or chronic overdrainage syndrome. I began to do considerable online research to explain the dura inflammation and increasing pain, cramping, and fatigue.
Then in June 2015, a one month planned trial of Prednisone serendipitously helped to shape an explanation for the dura inflammation. This 13-day trial (10mg/day week 1; 5mg/day week 2), led to my ventricles draining out with my Certas CNS shunt valve set at “2,” where it had been for the past 3 years. The “2” setting is the 2nd lowest of 7 settings. I immediately discontinued the Prednisone, and my Certas valve was raised up to “3,” where previously it had caused me headaches and cognitive difficulty. Since about 2012, my ICP had also become lower. In Feb. 2015, it was measured to be “1” cm H2O.
In October 2015, the dura inflammation was formally diagnosed as pachy meningitis. Methotrexate and Azithioprine were then separately given, but led to a hospital admission in January 2016 of sepsis and atrial fib associated with my kidneys. This led to an order for a muscle biopsy, and I was instructed to stay off Prednisone and similar drugs until after the biopsy. However, my only substantive relief so far has been Prednisone. And I went back on a low dose in the interim until the biopsy is scheduled.
Where’s the mHealth?
On February 12, 2016 – my health plan added to the confusion when they issued an authorization for my muscle biopsy with a 14 day window. But I have to be off Prednisone for 4-6 weeks. And I’m concerned about the recovery time from a deep cut into my right thigh while having balance difficulties and muscle cramping. Where’s the mHealth? Here’s one on my blogs on Design & Best Use of mHealth Apps.
In light of my considerable efforts since 1992, many have suggested I write a book. More recently, others suggested I become a TED Speaker. I’ve also been very innovative with drums and rhythms for health and brain enhancement. In fact, it was drumming that helped me overcome many of my challenges with hydrocephalus.
My Medical Experience
Since about 1998, I have been providing global online information on hydrocephalus and CNS shunt devices, initially as an FDA patient advocate, then as an mHealth inventer turned medical device consultant. In 1997, I designed & patented an mHealth app for hydrocephalus, the DiaCeph Test, that would run on a PDA. But I could never get funding or get past costly FDA regulatory hurdles to bring it to market. Prior to my 1992 auto accident, I spent 17 years as a nuclear medicine technologist where I owned my own company, Certified Nuclear Imaging, from 1982 to 1992. I had also provided instrument feasibility and regulatory affairs consulting.
Feb. 13, 2016 UPDATE
This update includes an Oct. 2015 diagnosis of pachy meningitis by my neurologist based on diffuse dura inflammation in my Feb. 2015 MRI with Gadolinium, my dramatic response to prednisone in June 2015, my CSF culture, and cranial nerve palsies.
My progress in global pain, cramping, fatigue, and cranial nerve palsies continued into October 2015. In November, my neurologist suggested I take methotrexate. Prednisone was doubled to 5 mg 3x per week. I soon suspected I has having intracranial hypertension per increasing headache. This was reported with methotrexate in the literature.
A repeat brain scan with Gadolinium was done Dec. 23, 2015 and revealed the dura inflammation to be improved and only remaining in spots. But there was evidence of increased ventriculomegaly beyond my Feb. 2015 baseline brain scan. The increase was thought possibly due to methotrexate and Certas valve at the higher “3” setting since June 2015. I was somehow tolerating the larger ventricles perhaps due to the immune suppressent meds. There was also quite a dramatic difference in ventricle size between the Dec. 2015 and June 2015 scans.
In further review of my brain scans on Dec. 28, 2015, dura inflammation can be seen on an earlier Feb. 2012 MRI with gadolinium, but was never reported. At that time, my only confirmed test results for an autoimmune disorder were for Hashimotos Thyroiditis. There had also not been any detailed CSF culture. Knowing of the dura inflammation then would have dramatically altered the course of my testing and treatment.




With evidence of new ventriculomegaly in my above Dec. 23, 2015 scan, methotrexate was discontinued and I was placed on azithioprine (50/100/150 mg). But in week 3, I began to experience chills and night sweats and presented myself to the emergency room, where it was discovered I had a sepsis coming from my kidneys. I spent two days in the hospital where my immuno suppressant drugs were discontinued. In follow up visits, my neurologist discussed the possibility of a mitochondrial disorder, and that it too would produce a dramatic CNS response with prednisone. So a muscle biopsy was proposed and is now being scheduled.
I frustrated and concerned with the number of mistakes in my care. I am told I need to be off all immuno suppresant drugs (i.e. prednisone) for at least 4-6 weeks before the muscle biopsy. But with so much pain and fatigue, I went back on low dose prednisone until a firm muscle biopsy date is set. I would also like to explore relief thru alternative medicine as I had excellent result in past years. I’ve written these blogs on Complimentary Medicine & Addiction and Nootropic Vitamins for the Brain.
Sept. 9, 2015 UPDATE
Without support from a rheumatologist or my neurosurgeon, I contacted a neurologist in India who published a paper on chronic overdrainage syndrome, and a neurologist in Philadelphia who authored a paper on chronic meningitis. Neither would comment.<
The medical literature on dura inflammation and chronic meningitis recommended oral corticosteroids, which included prednisone. I spoke again to the prednisone manufacturer who reiterated my dramatic response to prednisone was likely an anti-inflammatory mechanism. With that in hand, I discussed with my internist about trying a low dose of prednisone in an effort to try and manage my pain and fatigue levels. We agreed on 2.5 mg every other day and I started on it on Aug. 7th, 2015.
After 6 weeks on this regimen, I saw a 10-25% reduction in muscle pain & fatigue, cognitive challenges, and cranial nerve palsies (esp. swallowing difficulties). My Certas valve remained at a setting of 3, where 6 months earlier it produced cognitive difficulty. With the prednisone, I overall appeared to be doing better. One of my best gauges for optimal shunt setting is how I feel the instant I awake in the a.m.. I also factor in my daytime cognitive and productivity levels, which after 6 weeks on prednisone, were improving. I kept some notes of this in my phone.
Discussion of Dura Enhancement in my Feb. 18, 2015 Brain Scan
Dura enhancement was identified in my Feb. 18, 2015 MRI w/ contrast study. It can represent infection, inflammation, CSF leak or shunt overdrainage, malignancy, or meningitis. And meningitis covers a broad spectrum of disorders, from infectious meningitis, to non infectious or aseptic meningitis, that includes Lyme disease and autoimmune disorders. Further below, I include links to web sites of medical documentation on this.
Shunt infection was ruled out in February 2015 via CSF culture. As I have a CNS shunt for hydrocephalus, dura enhancement can also represent shunt overdrainage or intracranial hypotension (ICH). But in these cases (referenced further below), the ventricles become “collapsed.” By contrast, my ventricles have been above normal size since 2011, except for the 13-day prednisone trial and collapse of my ventricles in June 2015 – which was after the dura inflammation was discovered. The June 2015 MRI finding would indicate either an inflammatory process or non-infectious or chronic meningitis. Chronic meningitis could also cause my ICP to become low. In Feb. 2015, it was determined to be “1 cm” or 10 mm. My Certas valve has been at the “2” setting since March 2013, while my ventricles have been gradually enlarging. There is no evidence of shunt obstruction.
Overview of Meningitis at Merck Manuals
A number of non-infectious or aseptic menigitis disorders can cause low ICP and dura inflammation. I have also undergone 12 revisions, and in Feb. 2012 developed an abdominal rash or fungal infection following endoscopy for that complete revision. My February 2015 CSF culture also reveals an abnormal WBC count. SEE these slides below.
A one month trial of Prednisone was initiated on June 11, 2015, for pain management and stopped early due to headache and abnormal MRI: 10mg/day week 1; 5mg /day week. In terms of pain reduction, prednisone provided a lot of relief. But, I developed low pressure headaches on day 13, and an urgent MRI brain scan revealed that my ventricles had drained out and nearly collapsed. While trying to ascertain this dramatic effect on my CNS system, I spoke to the manufacturer twice, discussed it with physicians, and undertook a considerable amount of online research.
It does not appear that Prednisone measurably alters CSF production or clearance to the degree to collapse my ventricles in 13 days. The more plausable explanation is that prednisone is an excellent anti-inflammatory agent, and my inflammed dura was a ripe target. This vastly improved my CSF clearance which resulted in my ventricles draining out with my Certas valve set at “2.” An alternate theory is that a metabolic disorder is causing the dura inflammation with a similar response to the Prednisone. Now I’m faced with the challenge of selecting the right setting for my Certas valve, not knowing how long, or significant, the effects of the Prednisone might last. My Certas valve was raised from a setting of “2” up to “3” for now. Additional information on Prednisone can be found below.
July 9, 2015 UPDATE:

The decrease in the size of my ventricles on my 6.24.15 MRI brain after just 13 days of Prednisone (10 mg first 7 days, 5 mg next 6 days) was dramatic. What is unclear, however, are the factors which contributed to this dramatic reduction, and the identification of a possible systemic inflammatory process. Below, my two MRIs reveal a dramatic change in size after only 13 days of prednisone. SEE more MRI images further below.

Cadista’s labeling states prednisone can raise intracranial pressure (ICP). But would it cause more CSF outflow and reduce the size of my ventricles? After speaking to them twice now, it appears this mechanical action on CSF is minimal. If it were more an issue, I think we’d see more published on this in the hydrocephalus population.
My reduction in ventricular size could have been furthered by an inadvertent change in the setting of my Codman Certas valve. However, I have no cause to think it did. It was learned on June 25, 2015, the day after my MRI, that my Certas valve was at the lowest “1” setting, from a “2” setting on February 26, 2015. The setting was not checked before my June 25th MRI. So, it is possible the inadvertent change occurred in the interim months and contributed to the reduction in ventricular size. But I have no data to suspect it!
I think the more likely explanation is reduction of inflammation in “aseptic meningitis,” that can include fungal infections & auto-immune disorders, and may be related to my Dec. 2011 onset of Hashimoto’s thyroiditis, and more recent cranial nerve complaints. But there are many types of aseptic or chronic meningitis.
The next two links are manufacturer required labeling and warnings information. It is vague as to any effect in raising ICP. Prednisone has been in use since about 1950, and falls under the earlier limited regulatory framework.
http://www.cadista.com/product-listing.aspx?pid=47
http://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=931ceb82-23b9-46c6-a00b-4cd66ed6f88f
This next link is to an abstract on a study which reported how prednisone significantly lowered the production of CSF fluid in rabbits:
http://www.ncbi.nlm.nih.gov/pubmed/2553468
And the next link is to the FDA’s drug safety site, which does not provide any information.
http://www.fda.gov/Drugs/DrugSafety/
There has to be “hundreds” of patients with hydrocephalus who have taken prednisone over the years. Where is this data? This is what mHealth and data sharing can solve.
13 Day Trial/Event with Prednisone: (3) Preventable Failures
I offer the following critique since I have encountered so many failures in my care of the last 23 years. This is about preventable failures.
First, there should be more user information on prednisone with respect to CSF clearance in hydrocephalus. Apparently, it falls under older FDA guidance. Still manufacturers must act responsibly to provide information on the “health science of the times.”
Second, Codman released its Certas valve as MRI-safe. But from its subsequent recall and discovery of 0.6 percent suffering unintended reprogrammaing, it renders the Certas valve as “mislabeled.” And had I known this in 2012, I never would have selected for my Nov. 2012 revision. I would have selected the Miethke Gav valve. The Certas valve also “could” have contributed to the collapse of my ventricles in this Prednisone trial, if the setting were tripped earlier by some unknown magnetic field. In consideration, I would advocate suspect Certas valves be checked both BEFORE and AFTER an MRI – to rule out other interference sources of unintended reprogramming.
Third, Congress, the FDA, and the medical devices industry must act in good faith on the health sciences information of the times and modernize mHealth policy to allow for innovations in technology to help avert adverse prednisone and CNS shunt events. It seems quite clear that my experiences and poor outcomes would have been helped by better innovation, better data sharing, and more responsive FDA oversight.
I shared my user experience with the manufacturer of the prednisone, Prosar Corporation. I believe the addition of new mHealth information would greatly improve the efficacy and safety of this powerful, yet effective drug. The slide below lists some of its common adverse effects.

One additional step that may have been helpful in assessing the anti-inflammatory effects of prednisone, would have been to obtain an MRI with contrast – to compare to the earlier February 2015 MRI with contrast scan. From research and discussions with the manufacturer, I am learning my ventricular reduction was the prednisone retarding action on CNS dura inflammation, rather than any normal mechanical action on CSF. Next, I would like to rule out chronic overdrainage as a cause of my dura inflammation, and pose this Question:
Would there not be a different anti-inflammatory response of prednisone on inflammed dura in rapidly reducing ventricular size on MRI – in aseptic meningitis versus chronic intracranial hypotension or ICH? Wouldn’t there be a distinction? Which one also has more associated cranial nerve palsies? Which syndrome would you expect a more dramatic reduction on MRI? Answering these questions will help determine its etiology! Below, I provide two new studies on Intracranial Hypotension or ICH, and I offer additional studies in the section Medical Reference Studies on Dura Enhancement later in this blog. I do not feel (as my nsg does) that I have ICH. I feel my increasing global pain, muscle spasms, cranial nerve palsies, and low ICP are due to an aseptic meningitis.
Intracranial hypotension due to shunt overdrainage presenting as reversible dorsal midbrain syndrome
I can only speculate on how long the effect of the prednisone will last in retarding CNS inflammation, and in the best setting for my Certas valve. An mHealth or telesensor app for hydrocephalus would be helpful for logging this data. And a more definitive diagnosis would be helpful too. I used my earlier DiaCeph mhealth methods in determining that my ventricles had drained out, as documentation for ordering an urgent MRI.

My Certas valve was raised to “3” to counter any lasting effects of the prednisone. There has been discussion of raising it to “4.” But my experiences at these higher settings have proven to cause ventriculomegaly and cognitive difficulties. My neurosurgeon suggested I could revise my Certas valve to a more stable valve. But, I feel these other questions must be answerred first. I continue to search for answers, for more details on my case study, and complaints. Knowledge should be a good thing!
May 26, 2015 UPDATE
I have enclosed my February 2015 CSF fluid culture report below which reveals changes in my white cell count. These findings might indicate a non-infectious or aseptic meningitis. But there are quite a few aseptic and auto immune disorders matching my CSF culture & dura enhancement results. I’ve undergone 12 shunt revisions. But in my February 2012 complete revision, I developed an odd abdominal rash or possible fungal infection from the endoscopy portion of the abdominal fenestrations. This is seen in the photo below.

Could above Feb. 2012 rash have migrated onto the peritoneal catheter and into my CNS system – causing the dura inflammtion and low ICP?
At this juncture, my neurologist was split between a diagnosis of chronic overdrainage syndrome and aseptic meningitis. But my neurosurgeon it was chronic overdrainage. I felt it is aseptic meningitis. So my primary care doctor has ordered TB and Lyme disease tests, which were negative, and placed me on a trial of prednisone, which caused the CSF to overdrain thru my shunt and nearly collapse my ventricles – indicative of an inflammatory syndrome. Given all of the possibilities, I feel it critical to rule out chronic overdrainage and fungal infection from the prednisone trial results discussed above.

I had been taking the prescription medication patch Exelon for nearly 8 weeks, and showed obvious improvement in cognitive function. But my health plan does not cover off-label use. Exelon was FDA approved only for memory problems related to Alzheimers Disease and Parkinsons Disease. So it’s use in hydrocephalus is “off-label.” Today 20% of all prescriptions are off-label. Below, is a photo of my last Exelon patch, which I think exemplifies our country’s senseless rationing of medicine and innovation.

April 20, 2015 UPDATE
Exome Sequence (genetic) testing came back negative for neuromuscular disorder. But the results did not include incidental findings – and might possibly miss a related disorder if their keywords are not inclusive enough. The focus has shifted back to rheumatology and the significance of the “dura enhancement” on my Feb. 18, 2015 scan below, where I’ve learned it can represent several types of aseptic or chronic meningitis.
My Feb. 23, 2015, CSF culture also identified several abnormal WBC levels that may coincide with dura inflammation. I obtained the full report by going online at the new mHealth platform of Quest Diagnostics, but was only able to obtain my most recent lab report without having to pay a $9 fee for earlier reports.

My muscle cramping and fatigue complaints had been reported to my primary care doctor since 2009. And in 2015 I still have no answers. Clearly, new mHealth apps and changes in FDA regulations are needed in further today’s diagnostics and treatments. Below, I share more details on my experiences as a patient, patient advocate, and mHealth inventor.

Medical History
Since 1992, I’ve undergone 12 brain shunt revisions and numerous shunt malfunctions for hydrocephalus (1992 auto accident). That had been my primary health challenge until about 2012, when my shunt failed again, where I really felt fatigued and out of sorts, and was also diagnosed with Hashimoto’s thyroiditis. During that time, I began returning to bed in the middle of the day. My neuromuscular complaints of 35 years had been mild and managed well until 2011. And by Jan. 2012, I began to deteriorate and suffer more debilitating cramping, stiffness, and muscle pain, and bouts of hematuria, all of which then began occurring at lower thresholds of physical activity.
As Salvatore Iaconesi did in 2011, I put my case study online hoping for an open source medical cure. I prepared my brain scan images and case information as I have so often in my hydrocephalus consults (I provide global information on hydrocephalus). Prior to my 1992 injury, I spent 17 years as a nuclear medicine technologist, 10 of those years with my own company. Below, I also share details of my patient advocacy and public policy efforts, and my 17 year struggle to bring mHealth solutions to the care and treatment of hydrocephalus. I also put on drumming and drum circle events. I feel the availability of mHealth applications, such as my earlier DiaCeph Test for Hydrocephalus, would make a significant contribution to medical care and outcomes. Below, are my February 2015 brain scan images.


My Feb. 2015 MRI brain scan with contrast identifies “increased dura enhancement” diffusely spread over my brain and ventricular capsule. Dura enhancement can be caused by infection, inflammation, shunt overdrainage or CSF leak, aseptic meningitis, or auto immune disorder. In the past month, I’ve been undergoing further testing to try and determine the cause. A CSF culture was done to rule out infection, though it showed an abnormal white cell count. I presented myself to the emergency room hoping for new testing, and for radiology to review the above MRI scan and amend their report with additional findings. The dura enhancement MRI finding stands as “indeterminate.”
In my present case study, I seek expert input from neurologists, neurosurgeons, and neuro-radiologists that may lead to a diagnosis and treatment of my complaints. I was inspired by the story of the Italian artist and TEDx speaker, Salvatore Iaconesi, who put his medical case online, and it led to an open source cure of his cancer!
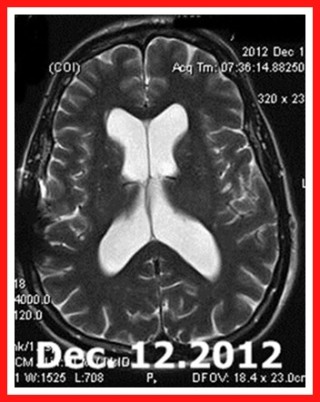
Experiences with the Codman Certas CNS Shunt Valve
My Nov. 2012 shunt revision to the Codman Certas valve was eventually optimized when the valve was set at 2, where it took 6 months of trial and error at different settings. My 2012 brain image above with still large ventricles was one month after surgery. My ventricular size and complaint reduction was achieved in part through monitoring with my DiaCeph Test paper forms and charts, and in email conversations and office visits with my neurosurgeon. This process would be much easier and more reliable (and cost effective) if there were an mHealth mobile phone or text app. It could be used worldwide.
History of Neuromuscular Disorder

On Oct. 13, 2016 I added the above 4-image childhood photo display showing drooping of the left side of my mouth, and perhaps left eye by age 16. My mouth drooping to the left has been pointed out repeated in recent years. So I sorted thru childhood photos to document when this began. According to the above photos, it was a “gradual onset” of facial palsy between ages 8-12. During those years, I was knocked unconscious for 5-10 minutes, suffered 2 different mouse bites, and a minor neck injury from sled-riding into a tree that I recall. I recall slowly developing physical limitations where I went from being the fastest and one of the toughest kids my age, to having a lot of difficulty running and playing sports.
At age 16, I suffered fainting episodes and was found to be very anemic, had onset of IBF (irritable bowel), and onset of sciatica in both legs. Visits to my family doctor during those years were unproductive. At age 20, I was advised to undergo reconstruction surgery of both knees by Dr. Noise, who was the Cincinnati Bengals head orthopedic surgeon and head of the Cincinnati General Hospital knee clinic. I never got the surgery. And later in California in 1980 at age 25, I was informed I had a peripheral neuropathy – per results of a muscle & nerve biopsy, and advised to get a desk job and discontinue sports.
In 1980, my neuromuscular complaints were primarily confined to my back and lower legs, which I learned to manage with exercise, nutrition, healing arts, and meditation, despite a bleak picture from my neurologist at that time. It is a long story, but eventually my personal health practices allowed me to overcome this ailment, and in 1981 led to overcoming most all of the disabling complaints and new healing and medical intuitive abilities detailed in this healing blog. For the next 11 years, I continued my health regimens up until my 1992 accident and onset of hydrocephalus. And after a couple years, was able to re-establish some level of routine to keep these complaints under control. In the photo below, I am age 34 and playing in a coach’s softball game with my son’s little league baseball. As you can see, I had become quite fit and muscularly developed despite the earlier 1981 diagnose – a surprise to all of my doctors. However, I faced continued episodes of IBF, anemia, and occasional bouts of (bilateral) sciatica.
In 1996, I learned some of my back pain was due to misaligned cranial faults per a very astute chiropractor. It was usually my left parietal cranial fault causing the back pain. In the years that followed, I learned to diagnose and adjust my cranial faults myself. In late 2012, cranial testing showed my entire head abnormal! I learned in 2015 I had pachymeningitis. To this day (Oct. 2016), it seems my global pain and cramping are related to my head, as I seem to get a little relief after adjusting my cranial bones.

It is unclear whether my present neuromuscular complaints are due to this earlier neuropathy, or to a new disorder. But it would seem related to neuromuscular complaints that date back to childhood. The global cramping, pain, and stiffness has worsened to the point that it compromises my daily activities. And cramping and post exercise hematuria now occurs at a lower threshold of exercise than 3-5 years ago. Since 2009, on at least two occasions, I have gone into kidney failure. And, on 15 or so other ocassions, I developed hematuria after hand drumming and treated myself at home with forced hydration.
Rhabdomyolysis vs. Metabolic vs. AutoImmune Disorder
I was initially diagnosed as suffering from rhabdomyolysis following 3-4 hours of heavy hand drumming on a hot evening that led to 25% renal function and hospitalization in Sept. 2009. I’ve had to scale back my drumming and other physicial activities since. And the cramping, pain, and stiffneess has become more problematic, that I simply am not able to do the level of physical activities I had done for many years. I also have new vestibular complaints thought due to right middle ear dysfunction, which can be auto-immune or cranial nerve. I feel this is related to the dura enhancement, hydrocephalus, and aseptic meningitis. The WBC findings in my Feb. 23, 2015, CSF culture would seem to support this as well.
Below is a published study on rust colored urine and hematuria following prolonged periods of hand drumming. However, this is reported during drumming over a period of many hours and days. Here’s the link:
Rust Colored Urine after Intense Hand Drumming
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2440284/
Clin J Am Soc Nephrol 3: 1022–1027, 2008
doi: 10.2215/CJN.04491007
As I have been helping others around the world with specialized information on hydrocephalus and CNS shunts, I am hopeful there is a scientist or physician out there who can explain my medical findings. The Power of the Internet: an open source cure!


Analysis of CT & MRI Brain Images
This Feb. 18, 2015, MRI brain scan image above reveals slightly enlarged ventricles when compared to the Aug. 2014 and Aug. 2013 scans. But, there is no comparison MRI with contrast to compare to the Feb. 2015 “dura enhancement.” MRI with contrast is not normally done in the routine follow-up of hydrocephalus. There is a limited MRI with contrast done on Feb. 12, 2012, during that month’s hospitalization and shunt revision. But the images are T1 images, and the 2015 study is the standard T2 Flair images of the dura. So it’s unclear whether the 2012 study is appropriate for comparison. Regretably, I could not get the radiologist to review, compare, and comment further on these studies. I’ve inserted these 2012 MRI with contrast images below.


My June, 11, 2010, brain scan image below was after revision to the brand new Low Pro Orbis Sigma II valve in Feb. 2010, which apparently had a specification problem. This Low Pro valve then drained my ventricles out in 4 months. And 2 weeks later, my shunt system obstructed and I began vomiting, and was again admitted to the hospital. Having experienced overdrainage, low intracranial pressure (ICP), and tiny ventricles several times before, I know what it feels like. I do not suspect overdrainage as the cause of my current MRI dura enhancement and complaints. But, I’d appreciate your feedback.

Medical Reference Studies on Dura Enhancement
Medical studies report that “increased dura enhancement” is associated with a number of medical sequel, including, low intracranial pressure, infection, aseptic meningitis due to the side effects of certain drugs, and auto immune syndromes and brain metastases.
Below, is a very comprehensive 2007 study of dura enhancement:
Patterns of Contrast Enhancement in the Brain and Meninges
http://pubs.rsna.org/doi/full/10.1148/rg.272065155
-see the EXTRAAXIAL ENHANCEMENT near top of the page
This next study on Medscape offers a concise overview of dura enhancement and its causes, but you must have a Medscape member login. It entifies MRIs of low intracranial pressure, and the (5) criteria typically seen to support the diagnosis:
http://www.medscape.com/viewarticle/467001
– Diffuse thickening of the pachymeninges with enhancement,
– Engorgement of dural venous sinuses.
– Enlargement of the pituitary.
– Subdural effusion / hematoma.
– Sagging brain stem
And yet another lengthy study on dura enhancement:
http://www.em-consulte.com/en/article/159231

Certas Valve Opening Valve Pressure Discussion
With respect to infection as a possible cause of my dura enhancement, a CSF culture was obtained and this was ruled out. However, during the shunt tap, my neurosurgeon commented that my ICP was low, about “1” in the supine posture, and lower than in past years. It gave him pause to consider raising the setting on my Certas programmable valve. But in my opposition to this, I shared how my headaches, cognitive complaints, and balance were “worse” when the setting was higher and my ventricles larger. It took quite a bit of trial and error shunt monitoring and trial settings with the Certas valve over 2 and 1/2 years to find that a setting of “2” was most optimal for me. In addition, it is perplexing how my ventricles have become larger in the past 2 years with the same Certas valve setting of “2,” and no evidence of shunt obstruction. This finding would also be present during infection or inflammatory processes. But what?
My Aug. 1, 2013, MRI reveals my smallest ventricles since the Nov. 2012 revision to the Certas valve. I agree there is some extracranial CSF outside the brain, but it also occurred in my 2008 scan when I felt great, and in my 2010 and 2011 scans when the shunts overdrained to tiny ventricles, though I didn’t feel horible as I do now. Unfortunately, we don’t have MRIs with contrast studies from those studies. So there’s no way comparing dura enhancement. But, the Feb. 2012 MRI study is post contrast, and could be used for comparison. But the radiologist did not review it for comparison.
Aug. 2013 is also the smallest ventricles I have had since my 2012 revision, and earlier Miethke Pro Gav valve in 2011 where my ventricles became tiny when the valve was turned down to 1 (similar to the 2010 Orbis Sigma valve image). During instances of overdraining, I usually knew it from my complaints. I was also able to verify it with monitoring from my DiaCeph Test. I did not find evidence of overdrainage with my present Certas valve setting of 2, either by my complaints, or DiaCeph monitoring.
About a year after my Aug. 2013 brain scan, I began to experience increased pressure complaints, and a visit to my neurosurgeon’s office revealed that my Certas valve had lost its setting and changed from 2 up to 3, most likely from a Nov. 2014 MRI brain scan (I did not have the setting checked after this MRI). Even though the valve was set back to 2, my ventricles today are incrementally larger than 2013, and my last scan in Nov. 2014, which I feel suggests an aseptic CSF space syndrome or inflammation. And now the Feb. 23, 2015, CSF culture seems to confirm this. But specifically what syndrome?
My brain scan image below reveals very large ventricles one month after an auto accident and initial diagnosis of hydrocephalus in 1992. I was 37 at the time.

My Global Outreach, Patient Advocacy, and mHealth for Hydrocephalus
As I shared earlier, I’ve been providing online information and support for the disorder, hydrocephalus, since about 1995. In 1996, as an affected user and patient advocate, I petitioned the U.S. Food and Drug Administration on unreported problems with Medtronic and Heyer-Schulte anti-siphon CNS shunts that dated back more than 10 years at that time. The following year, I designed and patented the DiaCeph mHealth monitoring method for monitoring of shunt malfunction in hydrocephalus. For DiaCeph, I created a weighted scoring method of clinical (complaint) markers that were specific to hydrocephalus and shunt performance.
When properly analyzed, DiaCeph data can give an accurate assessment of shunt performance and shunt malfunction. DiaCeph was also created in response to the false negative test findings associated with malpositioned (malfunctioning) Delta valves and anti-siphon devices. But eighteen years later, DiaCeph still remains on the shelf while the treatment of hydrocephalus and the lives of some two million Americans rests with 25 year old technology solutions. FDA and Congress have failed to allow new social networking and mHealth advances to go through, which would allow earlier reporting and intervention on problem medical devices.
My Original DiaCeph Test Markers (Parameters)

The diagnostic difficulties and false negative findings with anti-siphon shunts were also at the center of my 1996 petition to the U.S. Food and Drug Administration (FDA).
I suspected my poor outcome was being caused by my Delta anti-siphon shunt, and I spent more than a year researching and writing the FDA petition, and another year on the DiaCeph mHealth solution – all in an effort to get corrective medical care and proper outcome. But, I was denied this for nearly 5 years.
The unusual shunt malfunctions identified in my petition were termed “functional obstructions” by Dr. Higashi et. al. who published the critical scientific paper on the topic in 1996. Higashi described how it occured with Medtronic and Heyer Schulte anti-siphon shunt systems. I had two Medtronic Delta anti-siphon shunts between 1992 and 1998, and eventually I was able to show my DiaCeph Test that my Delta valve was operating as a higher pressure valve than its specifications stated. I also referenced hidden manufacturer pressure flow charts on the devices.
In the 3-year period it took to author the FDA petition, design the DiaCeph Test, and advocate for the 1999 STAMP Conference, I became thoroughly familiar with anti-siphon shunts, shunt malfunctions and diagnostics, FDA codes & regulations, mHealth technology that didn’t yet exist, and hydrocephalus advocacy – where I had to learn where my efforts were being opposed, and who was behind it. Even the FDA!
Studies indicated anti-siphon shunt problems were affecting about 2 out out of every 5 users. In examining how many of the shunts were sold between the mid-1980s and as late as 2007, I estimated the device failures affected 5,000-10,000 patients per year, or well over 100,000 patients over this period. These oversights and subsequent FDA failures, in my view, then paved the way for more device failures with programmable shunts, and at least two other CNS shunt devices. And there were specific individuals and organizations particularly involved in hiding these failures. My FDA petition (23 pages total) link below is to a PDF file on my web site, and also as a window on Slideshare.net.
“1996 Petition to FDA on Anti-Siphon Shunts w/ 1998 Ruling“
Why do I bring these experiences up? Because I feel neither the medical field, nor FDA, or any other group, properly addressed the issues that led to the earlier anti-siphon device failures. It took some 10 years for the FDA’s 1998 Ruling on my anti-siphon devices petition to become accepted science in the field. I believe the same poor QA (quality assurance) and FDA oversight that allowed these anti-siphon device problems to continue, led to problems with programmable shunts, an overall lack of progress with CNS shunts, and new chronic health problems in the hydrocephalus population today.
Hydrocephalus Care in U.S. compromised by Politics
1) Widespread failures with CNS shunts leading to a high incidence of surgical revisions, overuse of CT x-rays, and too many unexplained complications, physicians have come to accept poor outcomes in the treatment of hydrocephalus. As a patient advocate and inventor, I argue the problems are not in the patients, and not really with the shunt valves, rather, shunt valves with problems mfrs cover up! It leads to a lot of unnecessary confusion in care, and political views of poor outcomes rather than medical results; and
2) My managed care plan encourages physicians and facilities to cut and block care, and such practices are accepted as a part of the political practice of medicine. Similarly, in cases of widespread shunt device failures, physicians are discouraged in reporting these to FDA. And I believe if either I worked for the U.S. government, or an organization on the Obamacare exempt list, I would have a better plan and I might have a diagnosis and some treatment by now.
I have not included SS#, DOB, and other priviledged information – as are so often included and breached on medical sites today. I’ve just my health care!
I want readers to understand what I’ve been through in 23 years: 45 CT brain scans (and radiation exposure) and another 20 MRI scans, 12 shunt revisions (many of these surgeries were preventable), and the ill-effects of 75-100 shunt malfunctions.
Still – my story is nothing out of the ordinary. Some patients have had as many as 100 to 200 shunt revisions – and many CT scans, related radiation, and long term health problems due to device failures and poor FDA oversight.
Here are some of my more recent efforts to address problems in the care of hydrocephalus. In 2002, FDA had introduced new Post Market Surveillance for problem medical devices. I wrote to them with the required supporting guidance and asked them to apply this new guidance to CNS shunts. But, FDA denied my request as can be read in their letter below. Since then, there’s been a widespread increase in CNS shunt failures, which I believe is a direct result of FDA’s poor post market surveillance:
Stephen Dolle’s 2002 Request to FDA to include CNS shunts in New Post Market Surveillance
FDA’s David L. Daly’s Letter of Denial to include CNS Shunts in new 2002 Post Market Surveillance
My experiences in living with hydrocephalus, have often left me helpless and feeling more like a “prisoner” than a patient.
All this helped me to put my medical case study online. I also host two (2) case hydrocephalus studies from my global efforts on hydrocephalus. Two high profile neurosurgeons with close ties to the Hydrocephalus Association oddly took issue with my involvement and reports, and refused to read them, all while they routinely allow manufacturer’s representatives in surgery with their patients to advise on CNS shunt implantation. Plus, I take issue with neurosurgeons, who become aware of problems with CNS shunts, but do NOT report to FDA!
I have complained about manufacturers not reporting problems with CNS shunt devices to FDA, and the presence of reps in patient surgeries, then provides additional opportunities to “mislead” user surgeons on issues with their devices.
My involvement, monitoring, and reports, then helps offset any mis-information and confusion by device manufacturers, and provides important diagnostic data on CNS shunt performance and shunt malfunctions. I think the patient and family should decide whether my role is needed. And if so, their physician had better read my reports.
Hydrocephalus Consults explore mHealth & MRI Display Advances
In the first report, I created an algorithm to analyze the patient’s brain scans for signs of brain atrophy vs likely responsiveness to shunting. In the second report, I had the patient fill out paper forms with instructions that provided non invasive data on his condition and shunt performance. An mHealth app, if it were available, would accrue and direct the collection of this data, and help physicians in earlier and more accurate diagnosis, and earlier intervention and better outcomes in care.
Consult Report on Analysis of Brain Atrophy vs Responsiveness to Shunting in NPH
DiaCeph Monitoring Report of Patient with NPH
Today, there are no doubt thousands of hydrocephalus case studies similar to mine. It is estimated there are almost 2 million people in the U.S. today with hydrocephalus. And many more around the world. The advent of mHealth apps and social platform solutions would aid shunt monitoring and sharing of data on CNS shunt devices, greatly improving shunt outcomes. I would finish my Creative Brief on the DiaCeph Test App if I felt it might be produced and put into use. Let’s turn this around. Support mHealth!

Blog on Challenges of the Development of the Diaceph Test as a Mobile App
My Longstanding Web Pages on Hydrocephalus and CNS Shunts
http://www.dollecommunications.com/Shunt-Selection-Method.htm
http://www.dollecommunications.com/hydrocephalus-treatment.htm
I hope my papers demonstrate the possibilities of mHealth and open source sharing of medical information in the treatment of disease.
Outreach for Hydrocephalus
Poor reporting of problems with CNS shunts has led to an epidemic of poor care and outcomes in hydrocephalus, which has emerged as barriers to care and treatment – as I have shared. My launch and outreach with HydroPowered.org is but one way to combat this. In other instances, I feel we need not to be so tolerant.
In 2001, Fox Sports thought they’d use an ad campaign to exploit hydrocephalus, seemingly involving the Los Angeles Lakers and the Los Angeles Times.
The actor in the ad sported a Laker shirt while having a graphicly and grossly altered large head and caption that read, “It’s a lot to Absorb.” This was a full page ad in the Los Angeles Times.
I telephoned the LA Times, and then Fox Sports, and followed this up with letters. I felt their poor taste reflected a public disconnect with hydrocephalus, and lack of public awareness in poor outcomes. It was a low point for hydrocephalus.
In the months that followed, I shared my correspondence with Emily Fudge, then director of the Hydrocephalus Association. She promised to keep me in the loop. But months later, I realized I was misled and learned there was not going to be any outreach or appologies from Fox Sports. I suspect her organization received some money, however. This is the way it’s been. And this is why people like me need to speak out!

Further below, I am pictured in Washington D.C. for the 1999 STAMP Conference on Hydrocephalus, which I helped to bring about. Somehow, my DiaCeph Test was left out of the program – and I think that error contributed greatly to DiaCeph never being developed. After all, DiaCeph was conceived in response to false negative findings cited in my FDA petition, which FDA upheld. It is counter-intuitive for FDA not to support a solution to these shunt problems. And it was counter-intuitive not to invite the person to speak on the conference panel (me), who helped bring STAMP about, especially with all of my knowledge about hydrocephalus, my related petition research, innovations in shunt monitoring, and authoring of this important FDA petition.
It was FDA staff, Janine Morris, who I knew from numerous telephone calls concerning my efforts, and her boss, Larry Kessler, who then decided to withhold the FDA’s Sept. 1998 Ruling from the Federal Register – guaranteeing there’d be no news coverage of it – a move most unheard of, unless you’re Medtronic undergoing a major merger and $5B stock issue that month. That merger helped propel Medtronic and Sofamar Danek, and sealed the fate of 2 million Americans with hydrocephalus – assuring we’d face many more years of failed shunt devices.

1999 Article in the Orange County Business Journal

Article Page 2

Today, the treatment of hydrocephalus with CNS shunt devices, regulated by the U.S. Food and Drug Administration, is in shambles. There are other areas too, where FDA oversight is in need of immediate attention and modernization, such as the user information and data on older drugs like Prednisone, and the availability of mHealth devices and social network platforms, all of which will aid in the resolution of problems with drugs and medical device safety.
But unusually high incidence of CNS shunt device failures and related (failed) FDA oversight should draw scrutiny – and be investigated for misconduct. These failures date back to before my 1996 Petition in the FDA’s failure to act on significant problems with CNS anti-siphon shunts.
Since the FDA’s 1998 ruling on my petition and related 1999 STAMP Conference, there has been a significant increase in unreported problems with CNS shunts, many requiring shunt revision. The most notable of these has been with programmable shunts. My current Certas shunt is in this class, and was recalled in 2013 less than a year after it was approved. It is only the second of many shunts with problems to be recalled.
FDA Conference Agenda – 1999 STAMP Conference on CNS Shunts for Hydrocephalus
Stephen Dolle Paper of Recommendations: 1999 FDA STAMP Conference on CNS Shunts
I found the Hydrocephalus Assocation (now in Washington, D.C.) to be working with shunt manufacturers to avoid taking action on shunt problems, and to be working with FDA to not take any action, and that this relationship existed from 1996 to as late as 2013, and to some degree, still today.
The high incidence of CNS shunt failures led to poor progress in the care and treatment of hydrocephalus, and contributed to new health issues now being discovered from over-use of CT scanners, and new long term effects from an unusually high number of shunt revisions. I had discussed some of this with the renowned field inventor, John Holter, before his death. He and I were 100% in agreement.
No amount of money spent on research can fix these kinds of problems. As a patient and scientist, I am outraged. I’ve felt like a prisoner.
Below, I include information on Salvatore Iaconesi, who earlier placed his medical case online for open source care, and for his efforts and presentation at a TED Global event.
Salvatore Iaconesi’s 2012 TED Global Speech on Open Source Cure for Cancer
Salvatore Iaconesi’s Web Sites
http://opensourcecureforcancer.com/
(in Italian)
http://www.artisopensource.net/network/artisopensource/salvatore-iaconesi/

Tips and New Treatments in Managing Sound Sensory Processing Disorder
And for those of you who enjoy outreach with hydrocephalus, I have a fun site for hydrocephalus at http://www.HydroPowered.org that I hope you find uplifting. One of my main characters and hydrocephalus super-heroes is none other than the Terminator, who comes complete with a self-correcting brain implant.
Check out my super-hero stories and other content at HydroPowered.org

If you would like me to speak or consult on mHealth applications, innovation and product development in hydrocephalus, or share any of my experiences, please contact me thru DolleCommunications.com or StephenDolle.com.
If you have experience with hydrocephalus or non-infectious (aseptic meningitis), or neuromuscular disorders, I’d appreciate your feedback on my case study. As I share, I have been providing global informaiton on hydrocephalus since about 1995. I prefer science and innovation over politics and the status quo.
I also post my case study here in support of 2015 Brain Awareness Week at http://www.dana.org/BAW
I look forward to hearing from you.
Thank you.
Stephen Dolle
Contact[at] DolleCommunications [dot] com
Tel. (949) 642-4592




I continue advocate on behalf of hydrocephalus. I wrote this blog last month in support of rare diseases day. Link:
http://wp.me/poW1N-5a
LikeLike
Good luck with your search for a solution. This is a very helpful and informative paper.
Best wises, Andrew
LikeLike
Stephen, I am glad to have connected with you via LinkedIn and now to have learned your story. I have also posted at . I am guessing we are pretty close in age. I am 54. In your search for a “solution”, I hope you are successful in finding that solution which prevents the condition “in utero”! Philip
LikeLike
Philip, we are brothers connected thru the challenges of having hydrocephalus. Over the past 23 years, I have undertaken a number of efforts on behalf of hydrocephalus. But unfortunately, this has not been met with widespread support. While I advocate for more efforts in the prevention of in-utero hydrocephalus, I think my case study here calls attention to still unfair practices by insurance companies, better understanding of hydrocephalus thru brain imaging, and the need for mHealth solutions in the treatment of complex disorders like hydrocephalus.
LikeLike
I appreciate your efforts. We have a lot in common, I was diagnosed with normal pressure hydro and shunted 10 months ago at the age of 58, all in the matter of one week. I am also a scientist, a pharmacology professor specialized In renal pharm,toxicology and physiology. Like you, I feel compelled to understand what’s going on in my cranium and peruse the literature whenever I can.
LikeLike
Thanks for sharing. I find much of the literature to be lip service to FDA & device mfrs, rather than reporting the true outcomes. I suspect my current outcome is not an isolated thing, and that we’re likely going to see a lot of similar unexplained complaints in patients shunted for life or for many years (23) as in my case. However, I could have a secondary or unrelated auto-immune disorder. I am on a prednisone trial right now for this. I am also taking samples of Exelon & Namenda to help with memory. I think the field wishes to piant an overly positive picture of NPH outcomes. I believe many patients would be helped by meds like Exelon & Namenda, despite no supporting studies I could find. My response with Exelon was dramatic, and also reduced irritability. I will update this blog soon.
LikeLike
Thank you for posting your story, Stephen. I am only sorry you have to endure this condition as the result of a preventable circumstance. I am going to suggest “Exelon” to my neurologist who currently is treating me with “Aricept”, not for Alzheimers but for my working memory issues, effects from which I can never be certain.
LikeLike
Phil and my other fellow #hydrocephalus shuntees, #mindfulness and sports enthusiast, you are going to want to read my blog on the #science of #basketball where I share further (2/3 of the way) into this paper how compensatory #brain strategies came to me via #intuitive modalities to aid in #healing and #pain #management, and if it weren’t for things like what I do with #drumming and #basketball I don’t know how I’d survive http://wp.me/poW1N-8E
LikeLiked by 1 person
[…] https://dollecommunicationsblog.wordpress.com/2015/03/20/neuroscientist-puts-neurological-case-study… […]
LikeLike
[…] Complications of Hydrocephalus: A 2015 Case Study […]
LikeLike
[…] of my brain, termed pachymeningitis. Due to the complexities of this disorder, in 2015 I put up a Hydrocephalus Case Study on my health complete with brain scans and supporting medical […]
LikeLike
Question I was diagnosed with hydro cephalus and the neurosurgeon implanted a medtronic strata valve that was in 2014, last October of 2016 and early Nov My symptoms had returned and were rather exaggerated, We called the dr and his PA; they suggested we retrun to chgo immediately and they would squezze us in they felt the shunt was malfunctioning,We returned and the dr orderred x rays he stated the xrays showed all was fine and he adjusted the rate of flow, 2 nights later I was in real trouble rushed to emergency room where the dr did order a cat scan he immediately orderred a helicopter in that he found a significant chronic bleed subderal hematoma along with an acute bleed I was flown to chgo for surgery Now if my neurosurgeon would have done a cat scan a few days earlier along with of instead of just x rays he would have seen the subderal hematoma… What is the standard of care and did he do this wrong I am left with significant medical issues
LikeLike
John, I feel for you. Who did you see in their office during that 1st visit you disclosed a new problem? Were the x-rays done to check the setting of your valve? The fact that you suffered a bleed indicates the shunt setting was too low, OR, the shunt may have lost it’s setting to a lower setting – which could have led to the bleed. I certainly would want these questions answered. It’s hard to say whether your nsg breached the std of care in not ordering a brain scan. However, if your bleed and low setting were caused by your shunt losing its setting – that is something you might pursue. I think recovery from this is typically 6 months. However, in some cases there can be lingering problems. Find a nsg that you trust.
LikeLike